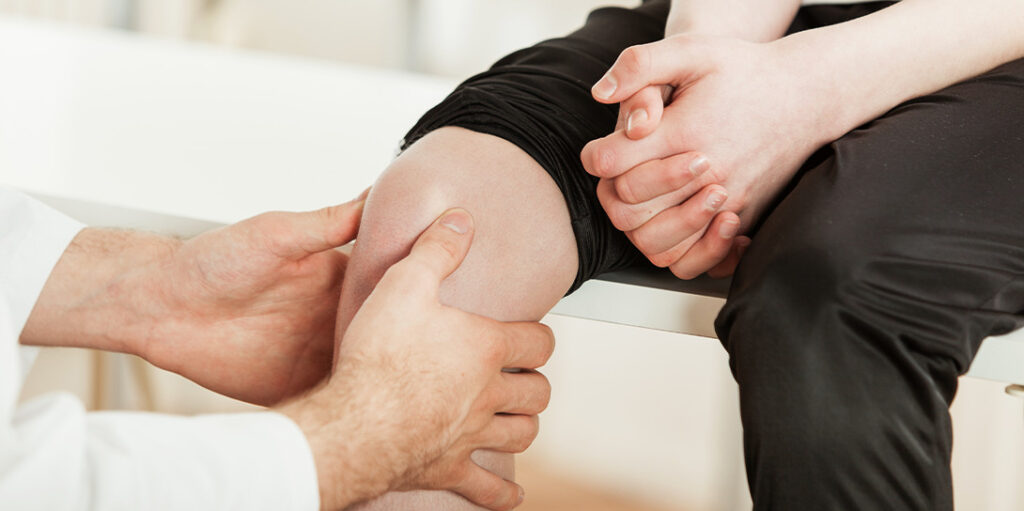
Articular cartilage is the smooth, white tissue covering the ends of bones where they meet to form joints. In the knee, this specialised tissue allows bones to glide smoothly against each other with minimal friction. An articular cartilage injury occurs when this protective layer becomes damaged through trauma, wear, or degenerative processes.
Unlike other tissues in the body, articular cartilage has a limited blood supply and poor self-healing capacity. Once damaged, it rarely heals completely on its own. Studies show that cartilage injuries affect approximately 15-20% of adults in Singapore, with higher prevalence among active individuals and those over 40 years old.