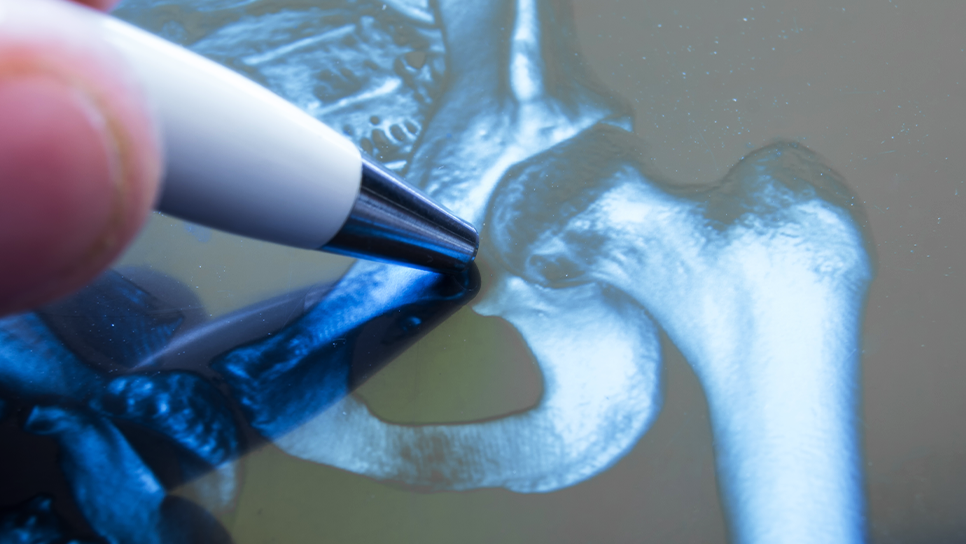
Femoroacetabular impingement occurs when abnormal bone growth causes friction between the hip ball (femoral head) and socket (acetabulum) during movement. This repeated contact can damage the protective cartilage and labrum, leading to pain and restricted hip motion. FAI is commonly seen in athletes and active individuals aged 20-40, though symptoms can develop at any age. In Singapore’s active population, FAI has become increasingly recognised as a cause of hip pain in younger adults. The condition often develops gradually, making early diagnosis crucial for preventing long-term joint damage.
Cam impingement arises from an abnormal bump or ridge on the femoral head-neck junction, which can prevent smooth rotation within the hip socket. It is more frequently observed in young athletic males and may result from repetitive hip flexion during adolescent growth years.