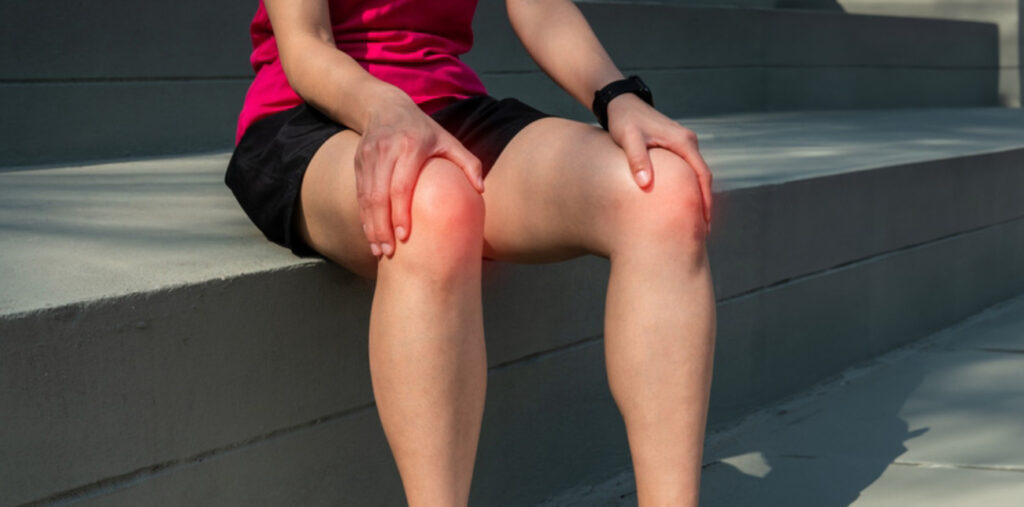
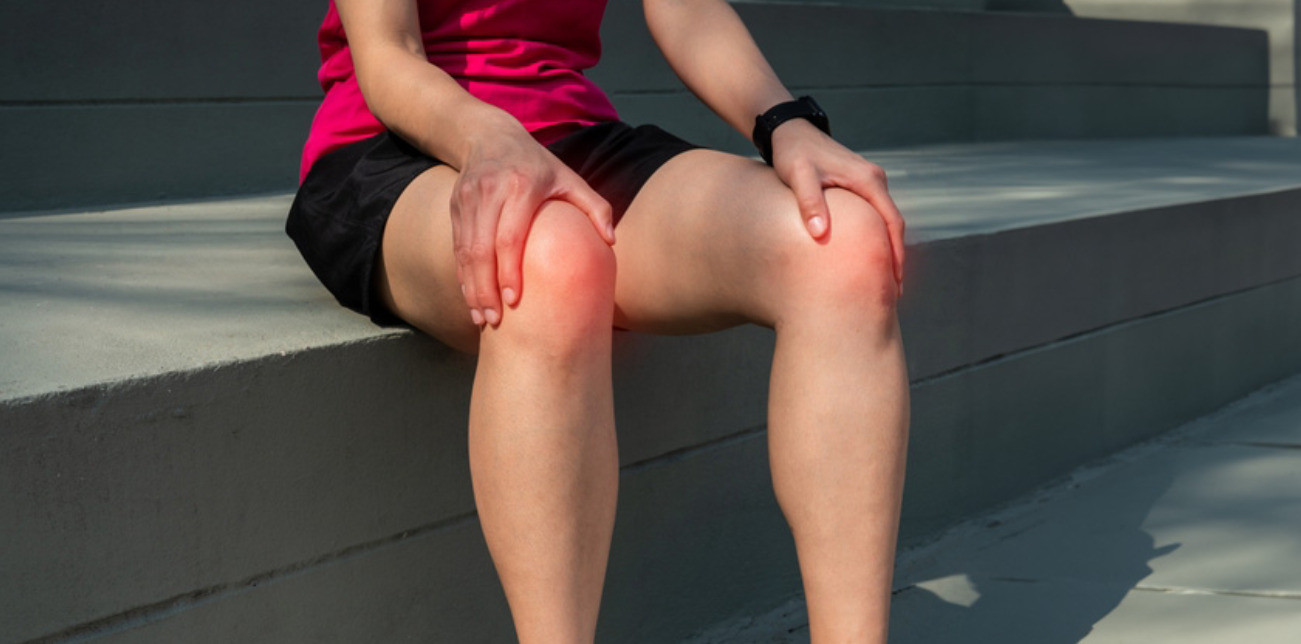
Knee tendonitis refers to inflammation or irritation of the tendons around your knee joint. Tendons are thick, fibrous cords that connect muscles to bones, enabling movement. When these tendons become overworked or injured, they can become inflamed and painful. Common forms include patellar tendonitis (jumper’s knee) and quadriceps tendonitis.
Knee bursitis involves inflammation of the bursae – small, fluid-filled sacs that cushion the knee joint. These sacs reduce friction between bones, tendons, and muscles during movement. When bursae become irritated or inflamed, they can swell and cause pain. The knee has approximately 11 bursae, with prepatellar bursitis (housemaid’s knee) being the most common type.