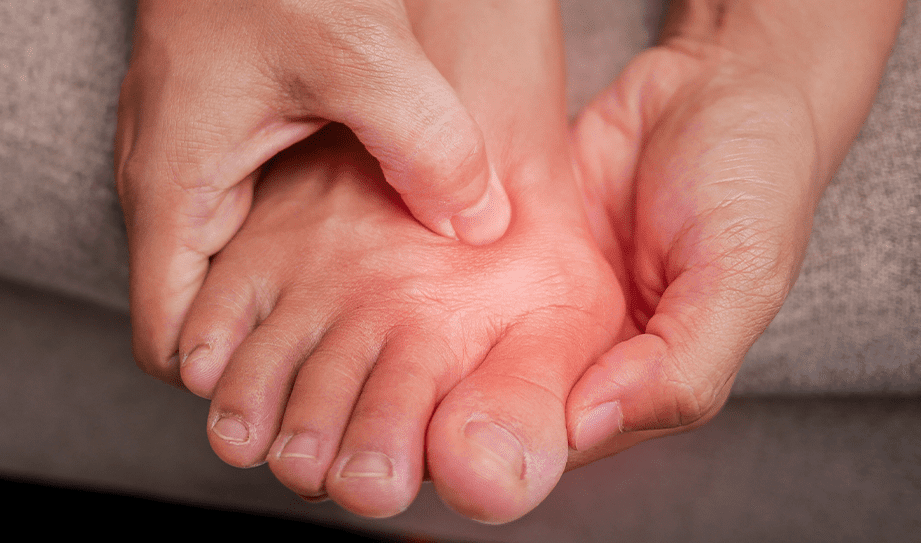
A bunion is a bony bump that develops at the base of the big toe when the metatarsophalangeal (MTP) joint becomes misaligned. This condition, medically termed hallux valgus, occurs when the big toe deviates towards the second toe, causing the joint to protrude outward. The resulting bump can become inflamed, painful, and may progress over time without appropriate management.
Bunions are a common condition that affects many adults, with prevalence increasing with age. Women develop bunions more frequently than men, often due to footwear choices and genetic factors.