Minimally invasive bunion and hammer toe surgery is a surgical technique that corrects foot deformities through small incisions, typically measuring just a few millimetres. Unlike traditional open surgery, this approach uses specialised instruments and fluoroscopic (X-ray) guidance to realign bones and correct deformities with minimal tissue disruption.
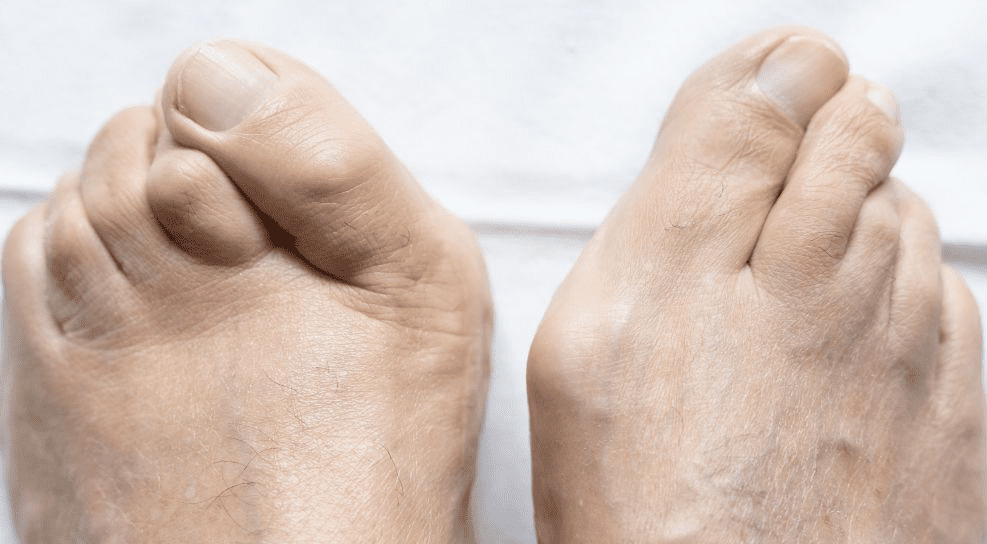
A bunion (hallux valgus) occurs when the big toe deviates toward the other toes, creating a bony prominence at its base. Hammer toe refers to an abnormal bend in the middle joint of a toe, causing it to curl downward like a hammer. Both conditions can develop simultaneously and often require surgical intervention when non-surgical measures do not provide sufficient relief.
During minimally invasive surgery, the surgeon makes precise bone cuts (osteotomies) to realign the affected joints. This approach addresses both the appearance and functional issues associated with bunions and hammer toes. The procedure typically results in less soft tissue damage, reduced scarring, and potentially faster healing compared to traditional open techniques.