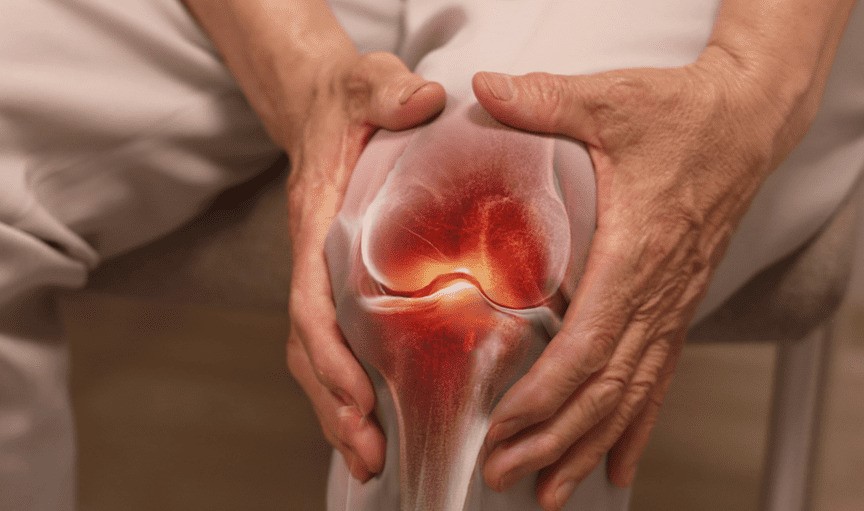
Osteoarthritis is a degenerative joint disease characterised by the gradual breakdown of cartilage, the protective tissue cushioning the ends of bones in the joints. As this cartilage deteriorates, bones begin to rub against each other, causing pain, stiffness, and reduced mobility. Unlike other forms of arthritis, osteoarthritis results from mechanical wear and tear rather than autoimmune processes. This condition most commonly affects weight-bearing joints such as knees, hips, and spine, though it can develop in any joint, including hands and feet.
Primary osteoarthritis may develop gradually without any identifiable cause, typically associated with ageing and natural joint degeneration. This type of osteoarthritis usually affects multiple joints symmetrically and progresses slowly over the years. Most patients with primary osteoarthritis usually begin experiencing symptoms after age 50, though the degenerative process may start much earlier.