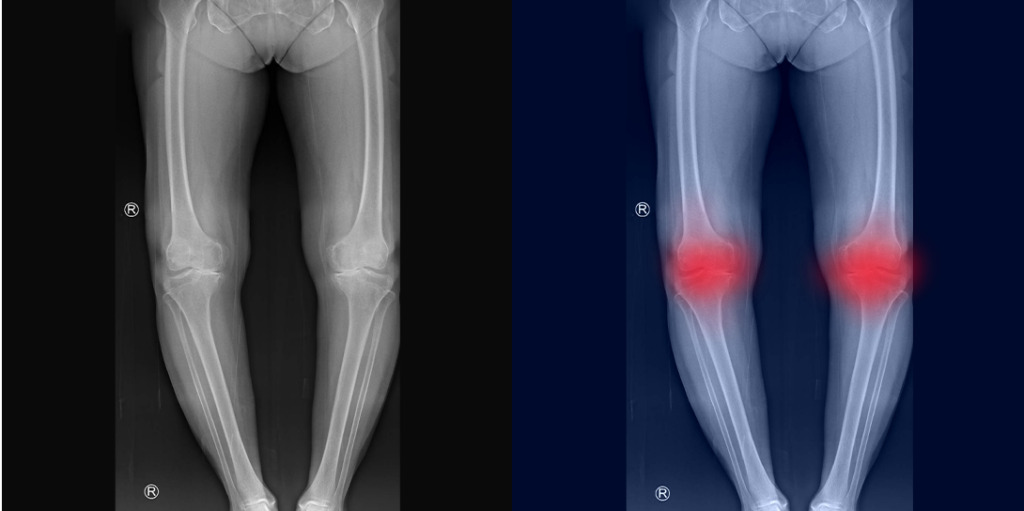
Bow legs is a condition where the knees stay wide apart even when the ankles are together, creating a distinctive bowed appearance of the lower limbs. The medical term “genu varum” describes this outward angulation of the knee joint. While some degree of bowing is normal in infants and toddlers up to age two, persistent or progressive bowing beyond this age may indicate an underlying condition requiring medical evaluation.
This is the most common type seen in infants and toddlers under two years old. It represents a normal variation in leg development that generally improves without treatment as the child grows. The bowing is usually symmetrical and mild, affecting both legs equally.