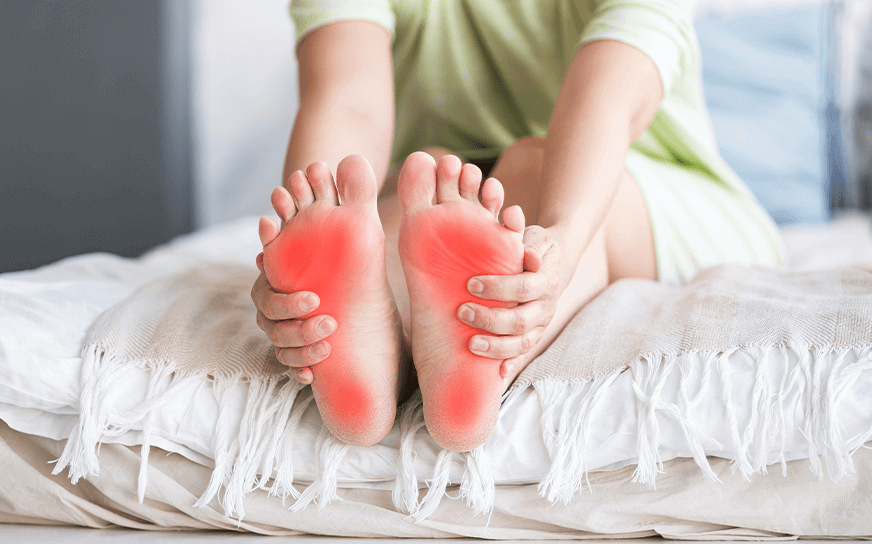
Plantar fasciitis is an inflammatory condition affecting the plantar fascia, a thick band of tissue that runs along the bottom of your foot, connecting your heel bone to your toes. This tissue acts as a shock absorber and supports the arch of your foot during walking and running. When the plantar fascia experiences excessive stress or repetitive strain, small tears can develop, leading to inflammation and pain.
- Sharp pain in the heel with first steps in the morning
- Heel discomfort after prolonged sitting
- Mild aching in the arch of the foot
- Slight stiffness in the heel area
- Pain that eases with light activity